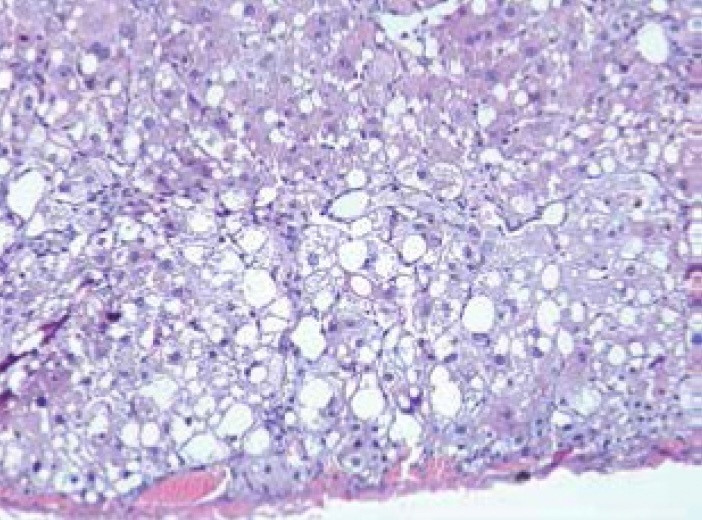
Liver cirrhosis remains a life-threatening condition characterised by fibrosis, architectural distortion, portal hypertension, and progressive liver failure. While liver transplantation is the only definitive treatment, donor organ scarcity and high costs limit access for many patients.
In an experimental study published by Pikirenia et al., researchers investigated whether spatially modulated erbium laser radiation could stimulate regeneration in cirrhotic liver tissue in an animal model.
The results suggest that microablative Er:YAG laser exposure activates regenerative processes in cirrhotic liver tissue without inducing thermal damage.
Study Objective
To evaluate the regenerative potential of cirrhotic liver tissue exposed to spatially modulated erbium laser radiation (2936 nm) using a microablative method in experimental animals.
Experimental Design
Mechanism of Action
The laser system used a Spatially Modulated Ablation (RecoSMA) attachment that converts the main laser beam into thousands of microbeams.
Instead of thermal destruction, the energy is transformed into:
Crucially, no coagulative necrosis or thermal damage was observed. The destruction mechanism was mechanical rather than thermal.
Key Findings
1️⃣ Early Phase (Day 1–7)
2️⃣ Regenerative Activation (Day 21–30)
Beginning on Day 21 and especially on Day 30, treated lobes showed:
Importantly, no regenerative changes were observed in the untreated right lobe.
3️⃣ Enhanced Regeneration with Repeated Treatment
Rats receiving a second laser treatment (30-day interval) showed:
The regenerative process was most evident on Day 30 after the second intervention.
4️⃣ Control Group
Animals with induced cirrhosis that received no laser exposure:
Histological Observations
Microscopy confirmed:
These findings indicate reactivation of regenerative pathways rather than scar formation.
Clinical Implications
The authors propose that spatially modulated Er: YAG laser therapy could serve as:
🔹 A regenerative stimulation technique
🔹 A fibrosis-modulating intervention
🔹 A potential bridge therapy before liver transplantation
By reducing fibrosis and stimulating parenchymal regeneration, this approach may prolong survival in patients awaiting transplant.
Why This Matters
Cirrhosis represents a condition where:
Current therapies largely manage symptoms rather than reversing fibrosis.
This study demonstrates that mechanical microablative stimulation can:
Without causing thermal damage.
Limitations
Nonetheless, the findings provide mechanistic insight into laser-induced tissue regeneration in fibrotic organs.
Conclusion
Spatially modulated Er:YAG laser radiation, applied via a microablative method, stimulates active regenerative processes in cirrhotic liver tissue in experimental animals.
Repeated treatments enhance neoangiogenesis, reduce fibrosis, and partially restore liver architecture without thermal injury.
These results support further investigation of this technology as a regenerative bridge therapy prior to liver transplantation.
Source:
Pikirenia II, Zemlyanik AN, Khomchenko VV. Possibilities of Liver Regeneration with Induced Cirrhosis at Exposure of Spatially Modulated Erbium Laser Radiation in Experimental Animals. Belarusian Medical Academy of Postgraduate Education
In an experimental study published by Pikirenia et al., researchers investigated whether spatially modulated erbium laser radiation could stimulate regeneration in cirrhotic liver tissue in an animal model.
The results suggest that microablative Er:YAG laser exposure activates regenerative processes in cirrhotic liver tissue without inducing thermal damage.
Study Objective
To evaluate the regenerative potential of cirrhotic liver tissue exposed to spatially modulated erbium laser radiation (2936 nm) using a microablative method in experimental animals.
Experimental Design
- Model: Liver cirrhosis induced in rats using carbon tetrachloride (CTC)
- Animals: 70 white rats
- Treatment:
- Left liver lobe treated with Er:YAG laser + SMA (Spatially Modulated Ablation)
- The right lobe served as the untreated internal control
- Radiation parameters:
- Wavelength: 2936 µm
- Pulse duration: 0.3 ms
- Energy density: 2.1 J/cm²
- Frequency: 3 Hz
- Microablation pattern: 50 × 50 × 50 µm
- Repeated treatments: Performed at 15 and 30 days in selected groups
- Evaluation timepoints: Days 1, 7, 15, 21, 30, 52, and 60
- Assessment methods: Histology, microscopy, morphometric analysis
Mechanism of Action
The laser system used a Spatially Modulated Ablation (RecoSMA) attachment that converts the main laser beam into thousands of microbeams.
Instead of thermal destruction, the energy is transformed into:
- Microablative zones (50 µm depth and diameter)
- Mechanical-acoustic waves
- Resonance effects within tissue
- Localised cellular micro-destruction
Crucially, no coagulative necrosis or thermal damage was observed. The destruction mechanism was mechanical rather than thermal.
Key Findings
1️⃣ Early Phase (Day 1–7)
- Existing cirrhotic features remained
- Localised destruction of individual hepatocytes in the treated lobe
- No thermal necrosis detected
- Treatment depth reached 5.5–6 mm
2️⃣ Regenerative Activation (Day 21–30)
Beginning on Day 21 and especially on Day 30, treated lobes showed:
- Reduced connective tissue
- Decrease in false lobules
- Endothelial proliferation
- Formation of new vascular beds (neoangiogenesis)
- Increased macrophage and fibroblast activity
- Proliferation of bile duct epithelium
Importantly, no regenerative changes were observed in the untreated right lobe.
3️⃣ Enhanced Regeneration with Repeated Treatment
Rats receiving a second laser treatment (30-day interval) showed:
- Stronger regenerative response
- More pronounced neoangiogenesis
- Greater reduction in fibrosis
- Improved structural restoration compared to single-treatment groups
The regenerative process was most evident on Day 30 after the second intervention.
4️⃣ Control Group
Animals with induced cirrhosis that received no laser exposure:
- Maintained classical cirrhotic features
- Showed no signs of spontaneous regeneration
- Displayed persistent fibrosis and inflammatory infiltration
Histological Observations
Microscopy confirmed:
- Mechanical micro-destruction of hepatocytes
- Absence of coagulation necrosis
- Reduction of portal tract fibrosis
- Decrease in connective tissue volume
- Restoration of the vascular network
- Reduction in false lobule formation
These findings indicate reactivation of regenerative pathways rather than scar formation.
Clinical Implications
The authors propose that spatially modulated Er: YAG laser therapy could serve as:
🔹 A regenerative stimulation technique
🔹 A fibrosis-modulating intervention
🔹 A potential bridge therapy before liver transplantation
By reducing fibrosis and stimulating parenchymal regeneration, this approach may prolong survival in patients awaiting transplant.
Why This Matters
Cirrhosis represents a condition where:
- Excess collagen deposition disrupts liver architecture
- Portal hypertension develops
- Hepatocyte function declines
Current therapies largely manage symptoms rather than reversing fibrosis.
This study demonstrates that mechanical microablative stimulation can:
- Trigger angiogenesis
- Promote hepatocyte regeneration
- Reduce connective tissue accumulation
Without causing thermal damage.
Limitations
- Preclinical animal model
- No functional liver tests reported
- No long-term survival analysis
- Translation to humans requires further investigation
Nonetheless, the findings provide mechanistic insight into laser-induced tissue regeneration in fibrotic organs.
Conclusion
Spatially modulated Er:YAG laser radiation, applied via a microablative method, stimulates active regenerative processes in cirrhotic liver tissue in experimental animals.
Repeated treatments enhance neoangiogenesis, reduce fibrosis, and partially restore liver architecture without thermal injury.
These results support further investigation of this technology as a regenerative bridge therapy prior to liver transplantation.
Source:
Pikirenia II, Zemlyanik AN, Khomchenko VV. Possibilities of Liver Regeneration with Induced Cirrhosis at Exposure of Spatially Modulated Erbium Laser Radiation in Experimental Animals. Belarusian Medical Academy of Postgraduate Education